Arthrosis of the shoulder joint is a chronic disease, caused by damage to cartilage tissue, followed by the appearance of bone growth and limited movement. Often, the elderly suffer, but physical processes and hard inflammatory processes contribute to the early development of pathology. Without timely treatment, movement in the affected joint is completely blocked.
General information
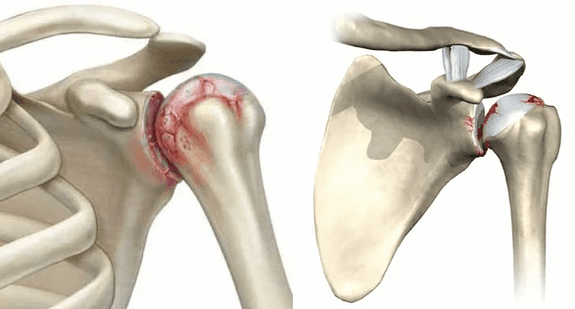
Cartilage is a fine layer between areas of bone in contact. This ensures easy sliding on each other, ensuring free and painless joint work. Excessive stress, inflammation or trauma can trigger a degenerative process that gradually spreads to the entire surface.
As a result, the smoothness of the articular surface is disturbed, and movement begins to cause pain. At the same time, bone growth begins to appear along the edges of the joint, replacing the affected cartilage. As the degenerative process takes place, it involves not only the bones, but also the surrounding tissues. Deformed limbs, muscle spasms, and ligaments become weak and lose elasticity. Without treatment, the person loses the ability to move the arm.
Views
Depending on the cause of development, primary and secondary arthrosis are distinguished. The primary form occurs spontaneously, most often against the background of excessive joint load. Secondary provoked by third -party pathology, e. g. , trauma, intense inflammation, metabolic disorders, etc. Both forms of the disease are similar in symptoms.
The reasons
Unlike the knee, ankle and hip joints, the shoulders do not experience significant stress when walking, which is why this form of arthrosis is rare. Pathology can be caused by:
- frequent excessive physical activity: weight lifting, professional sports, vibration;
- congenital abnormalities of the structure of the shoulder joint and adjacent structures;
- rheumatoid arthritis, systemic lupus erythematosus and other autoimmune diseases;
- congenital weakness of connective tissue, accompanied by hypermobility of the joints;
- injuries: dislocations, sprains and ruptures of ligaments, intra-articular fractures;
- hormonal changes and disorders (including pregnancy, menopause);
- inflammatory diseases of the joint and periarticular structures (arthritis, bursitis, etc. );
- metabolic disorders, including gout, diabetes mellitus.
An important role in the predisposition to arthrosis is played by heredity.
Degrees
The doctor identifies 3 degrees of deformed shoulder joint arthrosis, which determines the symptoms and treatment tactics options:
- Grade 1 is characterized by minimal manifestations: pain occurs only with vigorous or prolonged exercise and quickly passes after rest, and X-rays reveal subchondral sclerosis on the articular surface;
- with grade 2 arthrosis, the pain becomes stronger, one should use painkillers to make them feel better; radiographs showed significant narrowing of the joint space, extensive areas of cartilage destruction, as well as bone growth (osteophytes);
- Grade 3 disease is accompanied by persistent intense pain, very limited joint mobility, and pictures show complete destruction of cartilage tissue, deformation of bone structure and a large number of osteophytes.
Symptoms
The main symptoms of shoulder arthrosis include:
- pain: arises from a decrease in the smoothness of the articular surface, the growth of osteophytes and bone deformation; the intensity, duration and nature of the sensation depend on the degree of damage;
- cramps: one of the hallmarks of the disease, appearing at an early stage; differs in physiology with a rougher tone, and is also often accompanied by pain;
- movement limitations: associated with the appearance of pathological growths and destroyed cartilage particles in the joints; in the first stage, it is represented by a slight morning stiffness, then grows to immobility (ankylosis);
- deformity: changes in the first contour of only the joints, and then the hands, occur in later stages of the disease and indicate complete destruction of cartilage and involvement of bones, muscles and ligaments in the pathological process.
The development of symptoms can take years or even decades, but eventually arthrosis of the shoulder joint results in an inability to move the arm and severe pain.
Diagnostics
The diagnosis of shoulder joint arthrosis requires an integrated approach. To determine the diagnosis and determine the extent of the lesion accurately, doctors use the following methods:
- questioning and collecting anamnesis: patient complaints are recorded, the circumstances of occurrence of certain symptoms are determined; without fail, information on past illnesses and injuries, the presence of joint damage in the parents is clarified;
- examination: the doctor evaluates the joint visually, determines the distance of movement, the greatest pain zone, etc . ;
- X-rays and CT: the main diagnostic methods that allow you to see the symptomatic features of osteoarthritis (narrowing of the joint space, cartilage degeneration, bone growth and deformity);
- Ultrasound: makes it possible to assess the condition of cartilage, bones, ligaments, joint capsules and muscles;
- MRI: allows you to obtain virtual cuts of all structures of the affected area;
- laboratory diagnostics: blood tests reveal active inflammatory processes, which are often accompanied by arthrosis;
- arthroscopy: examining the joint from the inside with a camera inserted through a small puncture.
If the disease is secondary in nature, narrow specialist examination and consultation on the underlying pathology is mandatory.
Treatment of shoulder arthrosis
Treatment of arthrosis of the shoulder joint depends on the stage of the lesion: in stages 1 and 2, the disease can be successfully stopped or delayed with proper drug selection. With widespread destruction, the only way to restore mobility and stop pain completely is surgical operation - arthroscopy by "cleaning" the joint.
Drug treatment
Medical treatment for shoulder arthrosis aims to reduce symptoms and restore cartilage tissue. For this, the following groups of drugs are used:
- non-steroidal anti-inflammatory drugs: suppress inflammatory reactions and reduce pain; available in the form of tablets, ointments, suppositories and in the form of injections;
- hormonal agents (corticosteroids): used when NSAIDs are ineffective, have similar effects; good effect is given by prolonged drugs, injected directly into the joint cavity;
- antispasmodics, vitamin B: used to reduce muscle spasms that inevitably accompany advanced arthrosis;
- chondroprotectors: designed for long -term use, intended to restore cartilage tissue;
- drugs that increase microcirculation: indirectly stimulate the regeneration process by increasing blood supply to the affected area;
- enzyme blockers: slow down the partial destruction of cartilage tissue.
The selection of specific drugs, their dosage, frequency of administration and duration of the course is done only by a doctor! It is important to remember that self -treatment can cause accelerated joint degeneration and other side effects.
Physiotherapy
Physiotherapy techniques and physiotherapy exercises greatly facilitate the course of the disease and enhance the effects of medications. The following procedures have been shown to be effective:
- magnetotherapy: relieves pain, relieves inflammation, improves microcirculation and stimulates cartilage tissue regrowth;
- shock wave therapy: exposure to acoustic waves with a certain frequency contributes to the destruction of osteophytes, which facilitates movement in the affected joint;
- electrophoresis, phonophoresis: introduction of drugs (painkillers, chondroprotectors) into tissues using electrical impulses or ultrasound; promote better drug absorption;
- massage and physiotherapy exercises: dose load on the joints and strong manual action stimulate blood circulation in tissues.
Like medications, physiotherapy therapy, massage and exercise should be prescribed and carried out under expert supervision. If in quiet time they are beneficial, then the effect on the background of acute inflammatory processes can lead to an increase in pain.
Surgery
The last stage of shoulder arthrosis is accompanied by severe symptoms and requires surgical treatment. Most of the changes that occur as a result of degeneration are irreversible, which is why the only way to restore a person’s mobility is endoprosthetics. The affected joint is replaced with a modern prosthesis, which completely takes over its function. This surgery is very effective at young and middle ages, as it allows you to live painlessly for many years.
Prophylaxis
Like joint disease, shoulder arthrosis is easier to prevent than to cure. Orthopedists recommend following the following rules:
- exclude or reduce professional risk factors (vibration, weight lifting);
- does not allow hypodynamics, but also does not strive to record sports records: it is better to choose moderate training options;
- control diet and weight;
- undergo periodic inspections to identify possible problems.
Diet
With shoulder arthrosis in any degree, it is important to monitor nutrition:
- avoid overeating and being overweight;
- reduce harmful products: fatty, spicy, salty, alcoholic, canned foods, smoked meats;
- eat adequate amounts of collagen (meat jelly, aspic) and omega-3 foods (fatty fish, olive oil);
- prefer boiled, steamed or stewed foods, rather than fried foods;
- reducing the amount of carbohydrates that are quickly digested.
The diet should be complete and include the amount of vitamins, minerals and nutrients needed.
Consequences and complications
Even a little pain and soreness in the shoulder can be an unpleasant consequence. Without treatment, arthrosis leads to:
- significant limitation of movement until ankylosis (bone melting);
- severe pain even at rest;
- severe deformity of the shoulders and the whole arm.
To avoid this problem, it is important not to search on the Internet to find out how to treat arthrosis of the shoulder joint with folk remedies, but only contact an orthopedic specialist for the selection of therapy.
Treatment in specialized clinics
You may not be able to cure arthrosis on your own. Modern clinicians offer patients complex methods of treating shoulder arthrosis:
- modern drug therapy regimens that combine high efficiency and minimal side effects;
- time -tested and new physiotherapy techniques;
- PRP therapy;
- physiotherapy exercises and massage to relieve joint movement limitations.
If necessary, medical puncture is performed by introducing painkillers or artificial synovial fluid that facilitates movement.
We monitor patients throughout treatment to keep the disease under control.
The benefits of a modern clinic
Special blades offer their patients:
- a comprehensive health screening program;
- advanced examination for proper diagnosis;
- narrow expert consultation from various profiles;
- modern treatment regimens, including not only medications, but also physiotherapy, massage and exercise therapy;
- reasonable prices for all services.
Shoulder arthrosis is a problem that can change a person’s life completely. Do not let the disease enter an irreversible stage, come to consult an orthopedist.



































